Why is there a shortage of doctors and nurses in Catalonia?
Physicians mostly specialise in the same few areas and universities do not train enough nurses
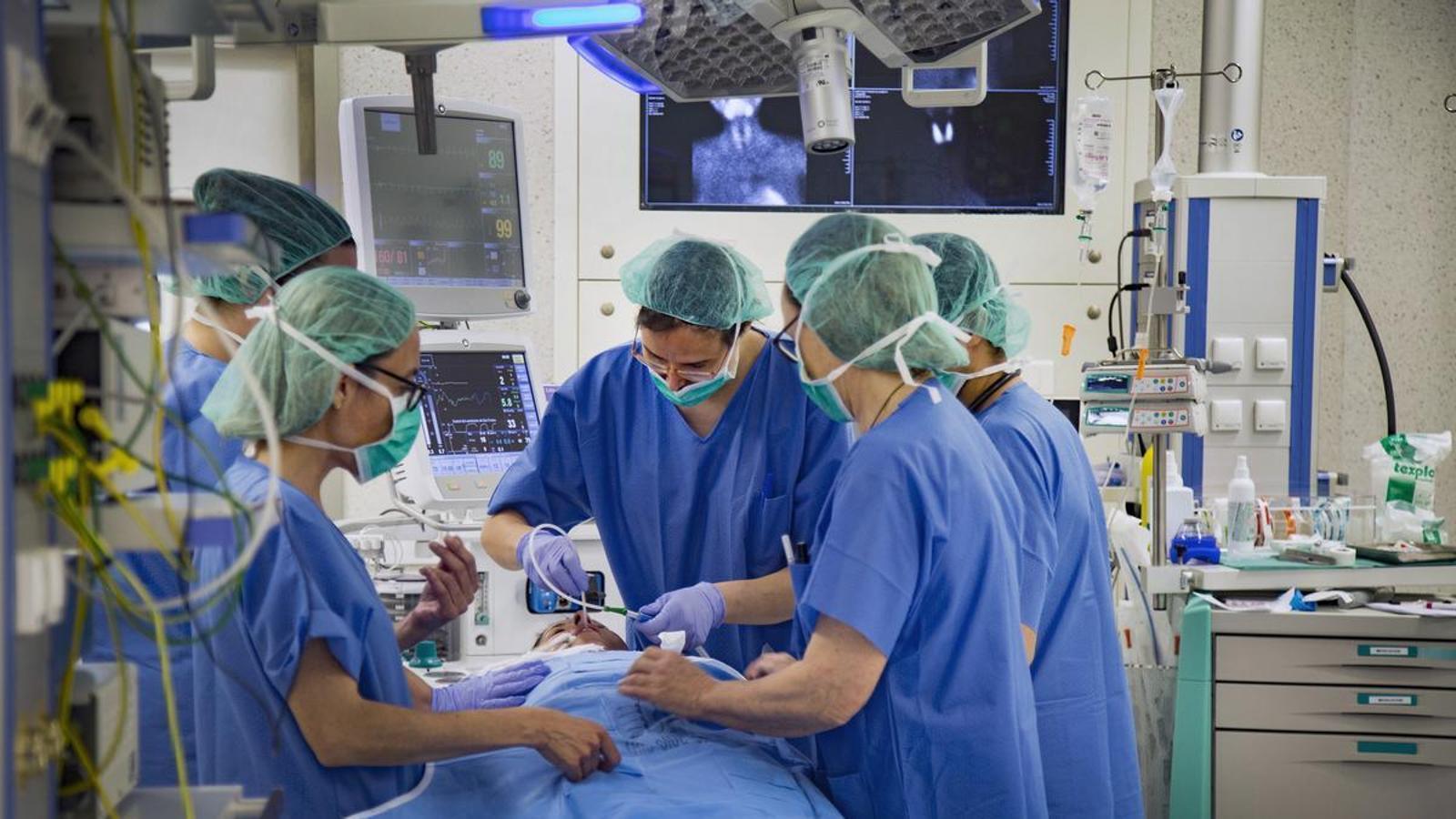

BarcelonaHospitals, both public and private, and primary care centres compete fiercely to recruit doctors and nurses. Their priority is to cover for the increasing number of staff on sick leave, as well as replace workers going on holiday. These professionals have been on the front line during the most dramatic moments of the pandemic. The problems is there are no more doctors and nurses to hire. And the professionals who are available will not accept the conditions offered to them, they are exhausted from stringing together temporary contracts or, having recently finished their training, they would rather start working when the summer is over.
The structural deficit of nurses and doctors has been dragging on for many years, but the current scenario is more worrying than ever. In 2021, 1,400 doctors and nearly 5,000 nurses were registered, an insufficient number to cover the needs of the system and ensure generational replacement, the cornerstone of professional planning. The rate of retirements is accelerating and the rate of training of new workers remains stable. This personnel crisis does not surprise the sector, which has been warning for years that it is the consequence of cutbacks and the rigidity of the regulations governing healthcare professionals, which constrain the administration, universities and healthcare centres when it comes to training and hiring personnel.
"We warned a decade ago that we would reach this staffing crisis and it will get even worse in four years' time, when 6,000 doctors from the baby boomer generation will retire and we will not be able to replace them," says the president of the Barcelona Doctors' Association, Jaume Padrós. The Association of Nurses also warns that the future looks bleak: in the next five years it is estimated that between 6,000 and 8,000 professionals will retire. Its president, Paola Galbany, says that the sector was relying on 1,700 nurses graduating to shore up services this summer in Barcelona alone and that the forecasts are not being met. "Before we had nurses but not enough jobs. Now we have too many jobs but we lack nurses. And many of those who do work do so in precarious conditions and without any kind of stability or are exhausted. How can we demand graduates work in these situations?" she denounces.
What is the origin of this shortage of healthcare professionals which could be unsustainable if immediate measures are not taken?
Universities
Lack of places on nursing courses and doctors going to work abroad
Healthcare careers are said to be the most vocational and, among them, medicine is king: every year it is the most demanded degree, with over 4,000 youngsters aspiring to fill one of the 1,200 places on offer. Only a quarter manage to get into the degree programme. Selection is based on grades, and the sector has long doubted that this is the best strategy. "Students who enter are not always the ones we are interested in as future doctors," says Padrós. Nor does the Generalitat believe that this should be the only criterion and advocates a prior screening that takes into account personal and non-scientific skills considered essential for a physician, such as empathetic communication or teamwork, by means of a personal aptitude test (PAP), like those future teachers have to take.
The single university district also has an influence, which allows any student in Spain to apply for admission to a Catalan university –or in any other region0 under the same conditions as its residents. Catalonia is the region that offers the most public places and, of the thousand graduates who finished last June, 30% came from other regions. "The problem is not that these doctors are trained in Catalonia, but that they will not end up working here," the sector explains. After graduating, most of them return to their place of origin but their governments have been spared paying for their training. "That is to say, they collect the investment made by the Generalitat. And the objective of a public university should be to guarantee the relay in the region that finances these studies," they add.
In the case of nursing, the problem is eminently the lack of places at university. Faculties cannot absorb the demand and not enough professionals are trained each year to guarantee retirees' replacement. This year the Departments of Health and Universities reached an agreement to increase the number of places to 2,745, nearly 600 more, starting next year. Eighty percent of these places will be at public universities. "The Government has made a good bet, but they should have increased them to a thousand. We would not saturate the market and if we want to increase the availability of hands for the coming years, these measures have to be taken now. It takes four to five years to train nurses," says Galbany.
Specialisation
There are not enough specialist doctors and nursing specialisations are not recognised
Another of the points the sector emphasises is the little room for manoeuvre the Generalitat has in health planning. The Law for the Regulation of Health Professions (LOPS) is more than twenty years old and grants the State practically all competencies for training and specialisation of doctors and nurses. "Not only is it necessary to work together on a new model for planning training places and criteria for access to degrees, but also to review LOPS and broaden the view of professional roles so that everyone can do what brings the most value," says the general director of the Catalan Union of Hospitals (UCH), Roser Fernández.
In the case of doctors, experts consulted consider the junior doctor system (known as MIR) works but can be improved. The supply of places was greatly reduced between 2011 and 2016, below 7,000 places, obeying the logic of cuts and, therefore, neglecting planning needs that should have been in place five or six years ahead, the time it takes to produce a specialist. In addition, junior doctors are concentrated in hospital specialities to the detriment of others such as family medicine. This year there were about seventy vacancies to become a healthcentre doctor, something that had not happened since 2014.
With nurses there is a problem of recognition. The vast majority have not got any specialisations because the current model does not give them any better working conditions than generalist nurses. In fact, 80% of nurses who have a specialisation are not Catalan and, in the medium or long term, end up leaving the country. The ministry only recognises seven specialisations but only midwives receive a higher salary (and by a European directive). In other specialities, such as mental health, geriatrics, paediatrics and primary care, steps are being taken but they are not yet recognised by collective agreements.
Precariousness
Temporary contracts, low salaries and too much bureaucracy
Paid training in exchange for a commitment to stay on at the position, higher salaries and even assisting workers' partners in finding work are some of the ways private healthcare providers seek to attract workers. The private sector also tries to attract professionals to nurture their workforce through economic incentives and different working conditions. "Every organisation has to know that in order to attract and retain talent they have to understand the value of new generations of professionals, who are looking to commit to projects that are attractive, worthwhile and where professional expectations fit in and where personal conciliation is respected," Fernández corroborates.
Hiring depends on each centre, but the healthcare system in general is too dependent on temporary contracts, especially nurses who can have dozens of temporary contracts, according to Galbany. "We have many nurses working as seasonal workers: in summer, in winter and, now because of covid, as reinforcements due to high numbers on sick leave. Nurses are not a wild card and they have to be taken care of," he exemplifies. As for doctors, Padrós claims that there is a shortage of professionals and, in the short term, he proposes making retirement age for doctors more flexible, to allow doctors who would like to continue working to do so.
Does the lack of personnel have anything to do with the brain drain that occurred during the worst years of the economic crisis? According to experts, it has an influence, but it is not decisive. Every year there are a hundred nurses who leave for other autonomous communities and even abroad, but there are also those who leave the profession (1,300 since 2020) because "they spend 10 or 15 years only working weekends, holidays and seasonal work," Galbany adds. Covid was the coup de grace. Some doctors also leave, but most do so because they return to their countries of origin or go on to Europe. On the other hand, Catalonia does attract new professionals from other areas: 49% of newly registered doctors and 35% of nurses come from outside Catalonia. In fact, the Health Department hired 600 Andalusian nurses in 2021 and in June it signed up 300 more from southern Spain.
This week the Spanish government approved a decree that will make it easier for 67,300 healthcare professionals across Spain with a structural position but a temporary contract to become permanent, 7,636 of them in Catalonia. This is a measure celebrated by the healthcare sector, but it is a reminder that its scope is very limited: the stabilisation will only affect Institut Català de la Salut (ICS) workers, but it will not affect the public-private healtchcare providers, which have a great weight in Catalonia. And the deficit in healthcare workers is structural, both in the public health system and in the private and public-private sectors. "The ICS has more volume and scope for managing people than subsidised centres, each of which is an entity in itself. But it is all part of the public health system and the professionals who work in subsidised centers should also be counted for seniority purposes," Fernández proposes.
